Search
Additional Topics
-

Recent study reports on Complications of vasectomy
March 25, 2025 -

Home-Based Semen Analysis
March 25, 2025 -

Has the Vasectomy Demographic Shifted?
March 25, 2025 -

History of No-Scalpel Vasectomy
December 15, 2023 -

Video Post More
December 14, 2023
The Vasectomy Techniques to Learn
Vasectomy has become widely adopted. This is partially because of the research efforts focused on improving the procedure's safety, efficacy, and patient experience. Advancements in surgical techniques, anesthesia, and post-operative care have contributed to reduced complications and faster recovery times. Learn about these innovative techniques in this section.

Video: Advancement in Vasectomy Techniques
In this video, Dr. Charles Monteith explains advanced techniques that make Vasectomy a safe and effective procedure with a low chance of failure. These steps include no-needle anesthesia, a no-scalpel skin opening, division with cautery, luminal coagulation, fascial interposition, and more.


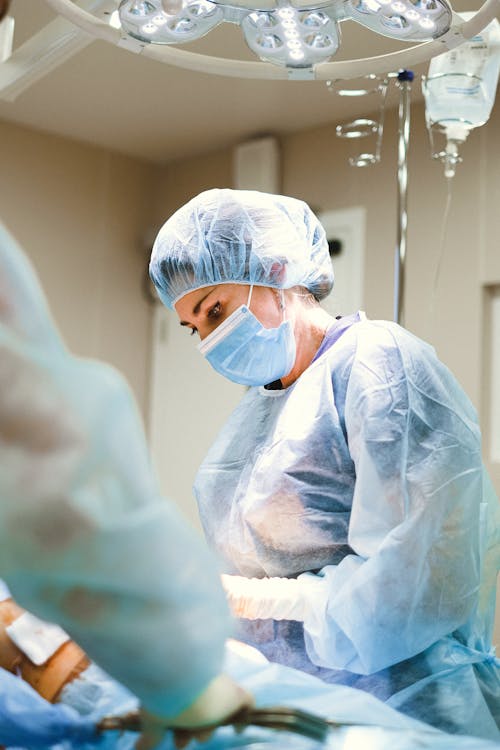
The Transformation of Vasectomy
The history of vasectomy reflects the power of scientific progress and societal evolution. From its controversial beginnings to its current status as a widely accepted and refined procedure, vasectomy has undergone a remarkable transformation. As healthcare providers, it is essential to acknowledge this rich history and continue to educate patients, dispel myths, and promote vasectomy as a safe and effective contraceptive choice for men.
The first documented vasectomy was performed by Reginald Harrison in the late 1800s. However, the early 20th century saw a concerning shift, as vasectomy was proposed as a eugenic measure for sterilizing individuals deemed “unfit” to reproduce, reflecting the era’s misguided beliefs and prejudices.
Over time, cultural stigma and misinformation surrounding vasectomy persisted, with many believing it would lead to physical weakness, sexual dysfunction, or a loss of masculinity.
.
No-Scalpel Vasectomy
Despite these challenges, vasectomy gradually gained traction as a contraceptive option, particularly in regions where family planning initiatives were prioritized. In the 1970s, a groundbreaking development occurred with the introduction of the no-scalpel vasectomy technique by Dr. Li Shunqiang in China. This minimally invasive approach significantly reduced procedural discomfort and recovery time, making vasectomy a more appealing choice for men.
No-Needle Anesthesia
About the year 1999 doctors began looking for a way to reduce the pain and anxiety associated with the use of a needle during vasectomy anesthesia. The results were what is known as the no-needle anesthesia technique. This is a minimally invasive approach to local anesthesia performed entirely without the use of a needle, as its name suggests. This approach has gained massive popularity due to its reduced operating time, less pain and swelling compared to traditional techniques.
Vasectomy Today
In recent times, vasectomy has become more widely adopted and research efforts focused on improving the procedure’s safety, efficacy, and patient experience have been done. Advancements in surgical techniques, anesthesia, and post-operative care have contributed to reduced complications and faster recovery times.
Today, vasectomy is recognized as a highly effective and safe form of permanent contraception, with failure rates as low as 0.1%. It is a widely accepted and accessible option for men who have completed their families or do not wish to have children.

No-Scalpel Technique Makes Vasectomy Safer and more Effective
Though the no-scalpel vasectomy (NSV) technique was developed in China in 1974, it began to spread outside of China in 1985.
Because of the inherent simplicity of NSV, it quickly came to be used in public health programs worldwide. By 2002, 37.8% of physicians, including urologists, family practitioners, and general surgeons, were using the NSV technique. Today, no-scalpel vasectomy has become the preferred method of male sterilization among healthcare professionals who perform vasectomies. The basic steps of the technique are as follows.
- Preparation: The patient is positioned comfortably, and the scrotal area is cleaned and sterilized.
- Anesthesia: A local anesthetic is administered to numb the scrotal area. In the case of a no-needle vasectomy, a device is used to spray the anesthetic on the skin, which feels similar to a mosquito bite. This minimizes the discomfort associated with multiple needle sticks.
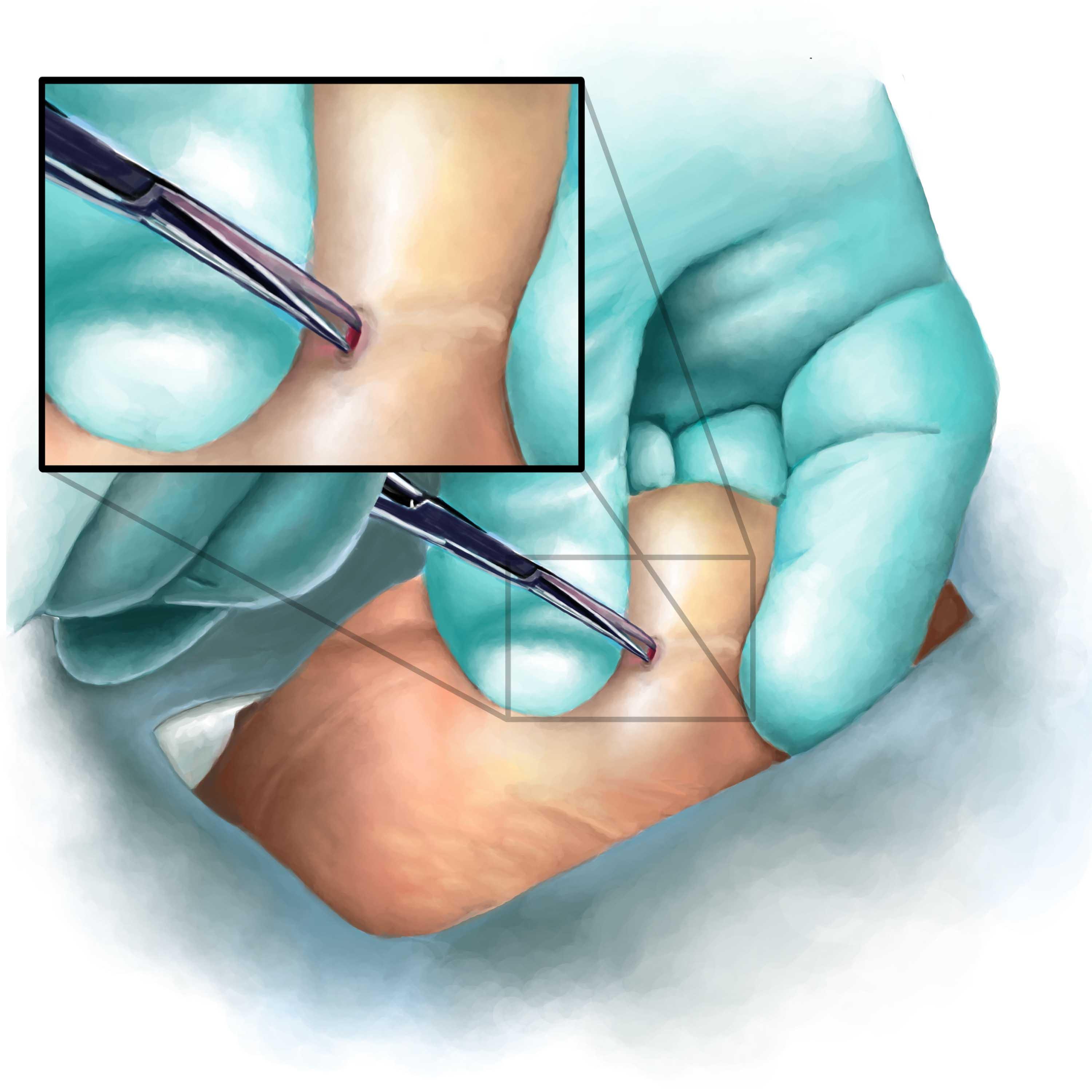
- Scrotal Puncture: A small puncture hole, typically about 1-2 mm in size, is made in the scrotum using sharp, pointed forceps. This instrument is designed to spread the tissue layers apart, allowing access to the vas deferens without the need for a scalpel or stitches.
- Vas Deferens Exposure: The puncture hole is used to access the vas deferens, the tube that carries sperm from the testicles. The vas deferens is gently lifted and stabilized using the same instrument, allowing for precise manipulation and minimal tissue trauma.
- Vas Occlusion: Once the vas deferens is exposed, a segment of it is removed or blocked to prevent the passage of sperm. This can be achieved using various techniques, such as cauterization, ligation, or the application of surgical clips.
- Closure: As there are no incisions that require sutures, the small puncture hole made in the scrotum typically does not need to be closed with stitches. The skin naturally retracts and closes over timee.
Equipment Needed
- Ringed Clamp
- Dissecting Forceps
- Straight Scissors
- Syringe / MadaJet
- 2% Lidocaine w/o epi
- Cautery / Ligatures
Benefits of No-Scalpel
- Minimally invasive procedure
- Faster recovery time
- Lower risk of complications
- Effective contraceptive method
The Recommended Technique
The American Urological Association (AUA) has recently released updated guidelines for healthcare providers performing vasectomy.
The guidelines emphasize the importance of minimally invasive surgical techniques, such as the no-scalpel vasectomy for reduced postoperative pain, faster recovery, and lower complication rates. Proper surgical technique, including adequate exposure and isolation of the vas deferens, is crucial for successful occlusion.
Postoperative care, follow-up visits, and semen analysis are essential to monitor for potential complications and confirm the success of the procedure.
Quick Recovery
Most men can resume normal activities within a few days.
Minimally Invasive
No-scalpel and no-needle techniques reduce discomfort.
Effective Contraception
Vasectomy is a highly effective form of birth control.
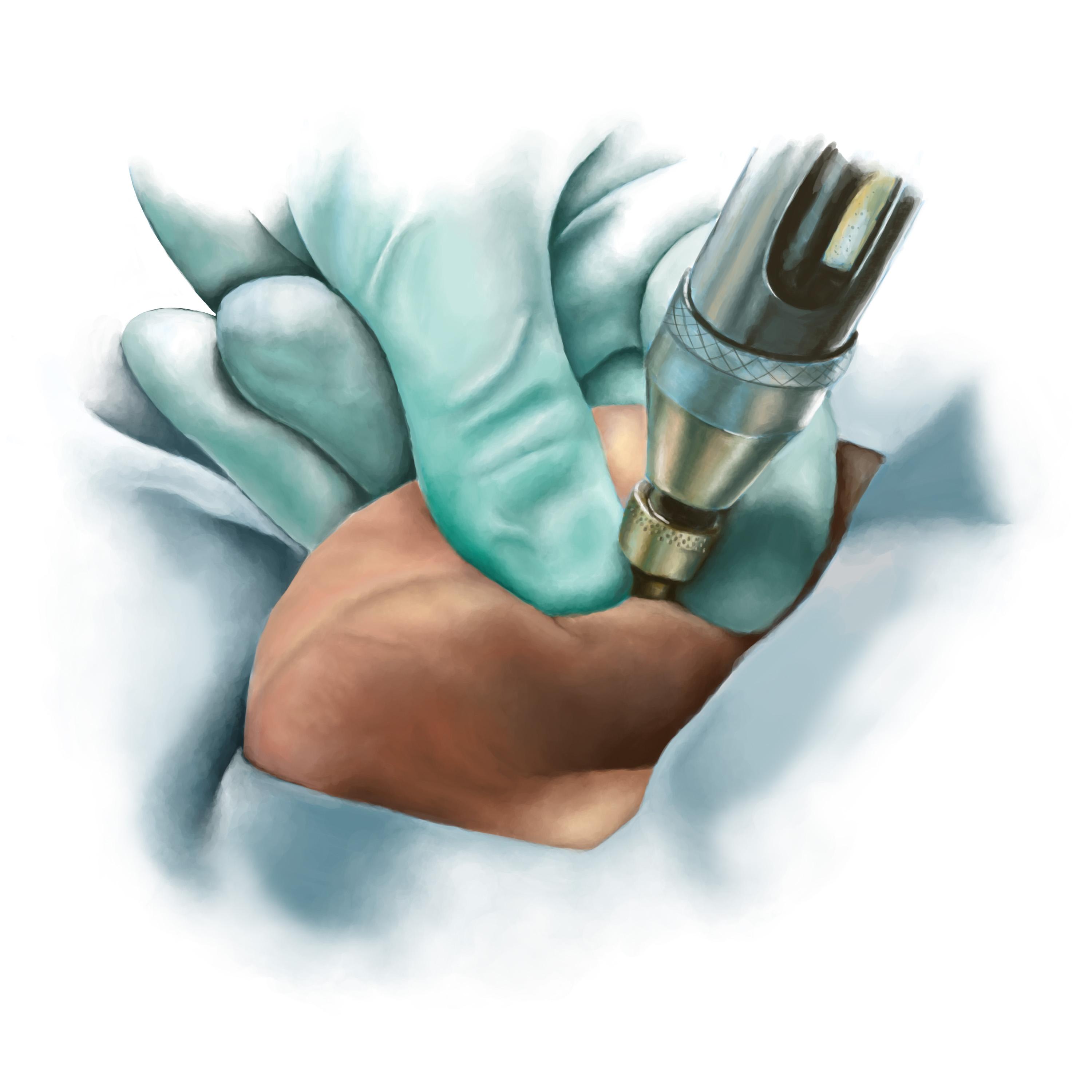
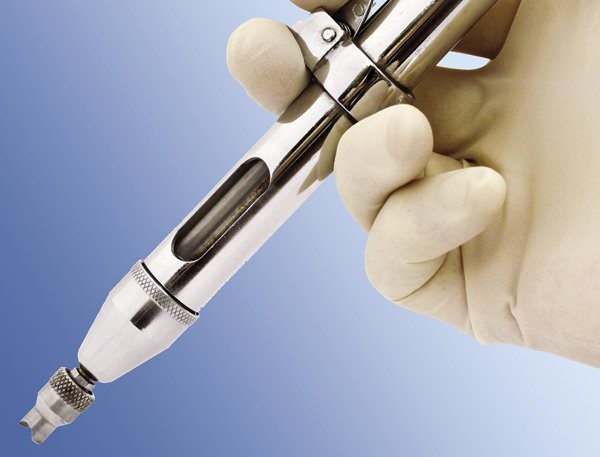
Eliminating the Pain Factor with No-Needle Anesthesia
The no-needle jet anesthetic technique using the MadaJet injector has revolutionized the no-scalpel vasectomy procedure, making it virtually painless and more appealing to men. This innovative approach eliminates the fear and discomfort associated with traditional needle injections for local anesthesia.
How MadaJet Works
The MadaJet is a medical device that delivers a high-pressure spray of local anesthetic solution directly through the skin, acting as a virtual needle. It creates a fine mist stream that easily penetrates the scrotal skin without requiring an actual needle. The anesthetic effect is almost immediate, within 10-20 seconds after injection, and more profound than that achieved by needle injections.For the no-scalpel vasectomy, 2-3 jet injections are delivered to each vas deferens, with a total of 4-6 injections typically sufficient for the entire procedure. The average volume of anesthetic solution per jet injection is only 0.1 cc, with 0.2-0.3 cc required for each vas.
Advantages of No-Needle
The no-needle jet anesthetic technique offers several advantages over traditional needle injections:
Eliminates needle phobia: Many men fear vasectomy due to the needle involved in local anesthesia. The no-needle approach addresses this concern, potentially increasing vasectomy acceptance rates.
Virtually painless: Patients experience only mild discomfort akin to a rubber band snap against the skin, with low pain scores reported during the procedure.
Rapid onset: The anesthetic effect is almost immediate, within seconds after injection.
Higher Patient Satisfaction
Studies report overwhelming patient satisfaction with the no-needle jet anesthetic method, reflecting its effectiveness and minimal discomfort.
By eliminating the needle and associated pain, the no-needle jet anesthetic technique addresses a significant barrier to vasectomy acceptance among men. Combined with the no-scalpel approach, which avoids the use of a scalpel, these refinements have made vasectomy a safer, less invasive, and more appealing option for male sterilization.
As healthcare providers, promoting awareness of these advancements in vasectomy techniques can encourage more men to consider this highly effective and permanent form of contraception. The no-needle jet anesthetic method represents a significant step forward in improving the vasectomy experience and increasing its accessibility to a broader population of men.
Vasal Occlusion Techniques for Vasectomy
In the realm of male contraception, vasectomy stands as a highly effective and permanent method of birth control. The procedure involves the occlusion, or blockage, of the vas deferens, the tubes that transport sperm from the testes to the urethra. Over the years, various techniques for vasal occlusion have been developed, each offering unique benefits and considerations.
Ligation and Excision
One of the earliest and most widely practiced methods is ligation and excision. This technique involves cutting and removing a small segment of the vas deferens, followed by tying or cauterizing the remaining ends to prevent the passage of sperm. While effective, this method carries a higher risk of complications, such as granuloma formation and potential recanalization (the re-establishment of the vas deferens).
Mucosal Cautery

Mucosal cautery, also known as electrocautery, is a more recent technique that involves cauterizing the inner lining (mucosa) of the vas deferens. This method aims to create a physical barrier and promote scarring, effectively blocking the passage of sperm. Mucosal cautery has been associated with a lower risk of granuloma formation and potential recanalization compared to ligation and excision.
Fascial Interposition
Fascial interposition is a technique that involves separating the cut ends of the vas deferens and interposing a barrier, typically a segment of the patient’s own fascia (connective tissue). This method creates a physical barrier and promotes scarring, further reducing the risk of recanalization. However, it is a more complex procedure and may require additional surgical expertise.
Medium Surgical lips

In recent years, the use of clips and implants has gained popularity as a minimally invasive approach to vasal occlusion. These devices are designed to clamp or occlude the vas deferens without the need for cutting or cauterizing. While effective, there is a potential risk of dislodgement or migration of the clips or implants over time.
The American Urological Association (AUA) recommends the use of techniques that minimize the risk of recanalization and granuloma formation, such as mucosal cautery or fascial interposition. Additionally, the AUA emphasizes the importance of proper surgical technique, follow-up semen analysis, and patient counseling to ensure the long-term success of vasectomy.
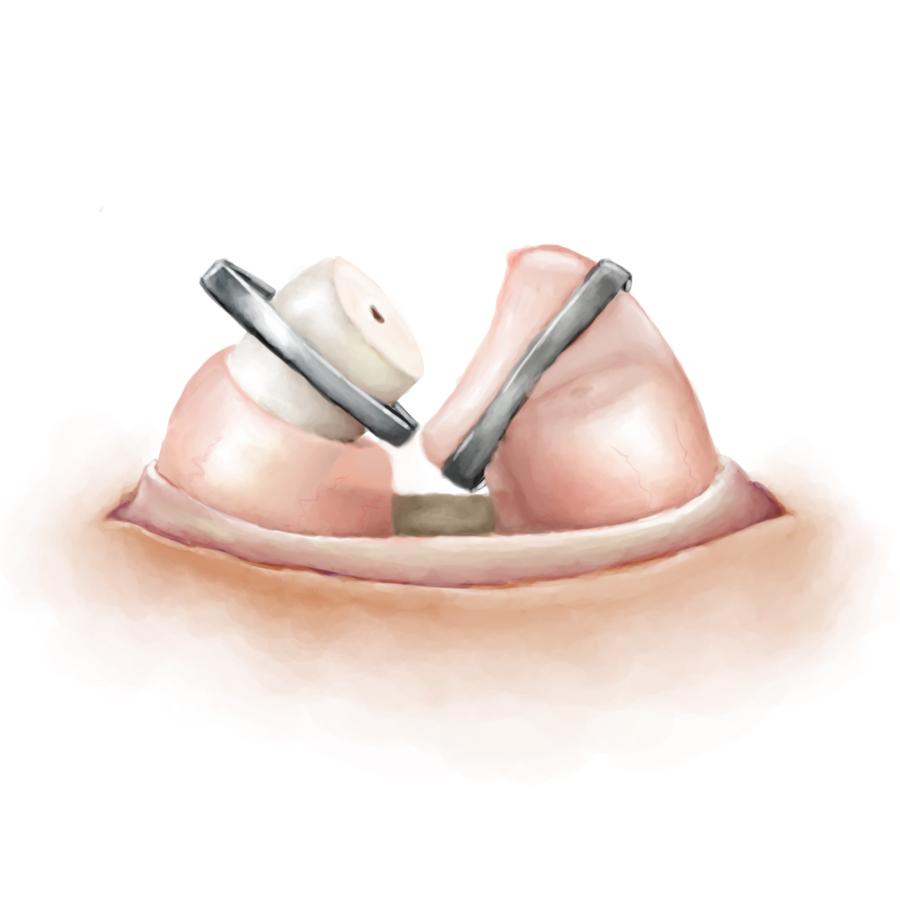
Minimally Invasive
Techniques like clips and implants offer a minimally invasive approach to vasal occlusion.
Reduced Complications
Methods like mucosal cautery and fascial interposition aim to minimize complications such as granuloma formation and recanalization.
Proper Technique
The AUA emphasizes the importance of proper surgical technique and follow-up to ensure long-term success.
Hands on Vasectomy Training
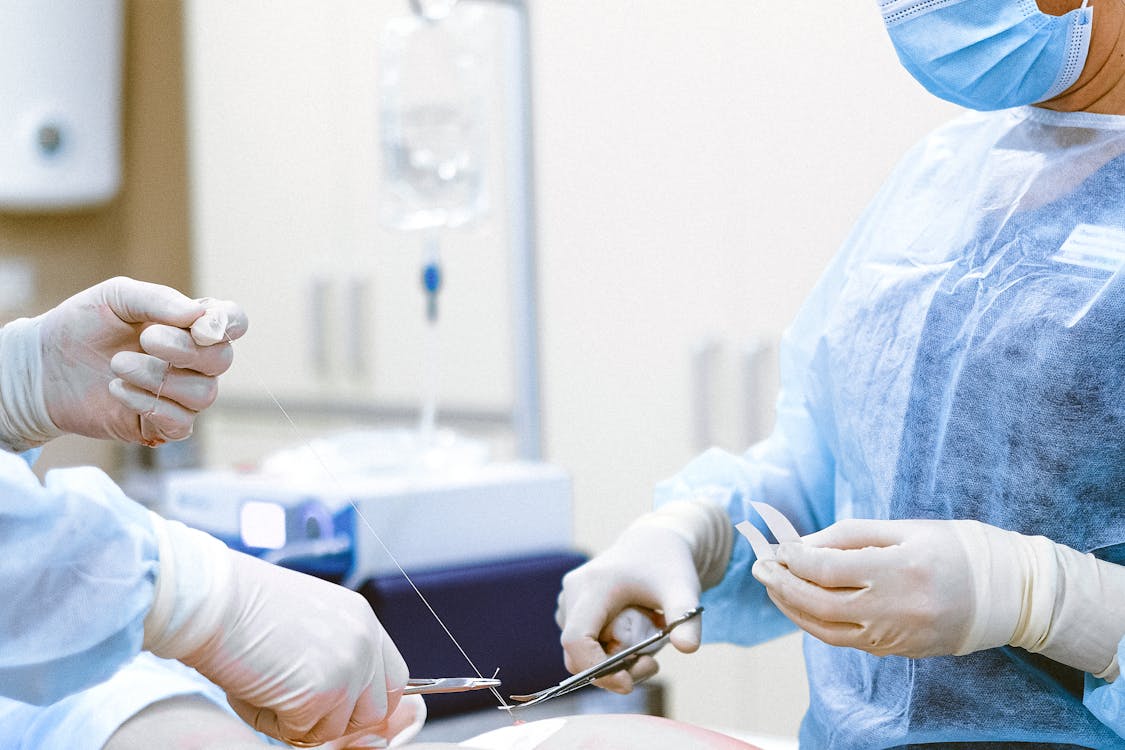
Hands-on training is crucial when learning to perform the No-Needle technique. While written presentations and video demonstrations are valuable, they cannot fully replicate the nuanced tactile feedback and real-time decision-making required during the procedure. Direct supervision by an experienced practitioner allows trainees to refine their technique, learn proper patient positioning, and master the precise handling of the MadaJet injector to achieve optimal anesthetic distribution without needle penetration.

Dr Douglas Stein
Florida, USA

Dr Charles Monteith
North Carolina, USA

Dr Nei Pollock
B.C, Canada
Dr Raj Selvarajan
Queensland, AUS

